|
8/28/2023 0 Comments Subchondral sclerosisLarge joint involvement is seen later in the disease. RA is more common in women and typically begins in the small joints in the hands and feet, usually with a fairly symmetrical distribution. It is recognized that both ultrasound and MRI are more sensitive than clinical assessment for identifying synovitis. The diagnosis of RA is based on clinical findings, along with laboratory assessment (inflammatory and immunological markers) and radiological assessment. Joint damage, including cartilage loss and osseous erosion, is thought to be mediated through synovitis there is strong evidence that synovitis is a predictor of future joint structural damage. This has led to an increased role for advanced imaging modalities such as MRI and ultrasound, both for earlier diagnosis and for monitoring the response to treatment. To achieve such remission, DMARDs need to be introduced early in the treatment pathway before structural joint damage occurs. These can induce remission and prevent the severe joint destruction that was commonly seen prior to their introduction. This autoimmune condition is mediated through inflammatory pathways, and its treatment has changed greatly in recent years with the advent of disease-modifying anti-rheumatic drugs (DMARDs) based on biologic therapies. Extra-articular inflammation, including tenosynovitis, soft tissue (rheumatoid) nodules, and multisystem involvement outside the musculoskeletal system (such as rheumatoid lung disease) may also be seen. Rheumatoid arthritis (RA) is an example of an inflammatory arthritis associated with joint inflammation characterized by synovitis. Erosive OA primarily occurs in postmenopausal women. There may be clues to the inflammatory nature of the disease from the clinical assessment, but the diagnosis of erosive OA is based on the imaging findings. While large joint disease may rarely be seen with this form of OA, it typical affects only the distal and proximal interphalangeal joints of the hands. It is important to realize that OA can co-exist with other forms of joint disease.Įrosive OA represents a subset of OA characterized by prominent inflammatory features including destructive joint changes in the form of osseous erosions. A wide variety of causes are recognized, but the radiological features at any joint may be identical to those of primary generalized OA (Table 11.1). In contrast, secondary OA describes cases where an underlying cause exists. It most typically affects the hands, thumb bases, hips, knees, and first metatarsophalangeal joints in the feet. This is more common in women and carries a genetic predisposition. The term primary generalized OA refers to OA when it occurs without an apparent underlying cause. However, OA has a complex etiology with multiple factors playing a part including genetics, race and ethnicity, obesity, age, and gender. This may come about through trauma to bones or ligaments or through altered ability of the tissues of the joint to transmit forces, for instance, alterations in the composition of cartilage in ochronosis or ligaments in some collagen disorders. The disease can be considered to arise primarily from a failure of the normal transmission of forces across a joint. Despite being so common, its etiology is still poorly understood and the subject of considerable research, much of it involving imaging studies. Osteoarthritis (OA) is the most common arthritis encountered and is seen in the majority of people at some stage in their lives. 
We will look at arthritides in three main categories: osteoarthritis, inflammatory arthritides (rheumatoid arthritis and spondyloarthritis), and crystal arthritides. KeywordsĪ wide variety of conditions affect the joints of the body, but for this chapter we will focus on the most common conditions seen and their imaging features. While cross-sectional imaging modalities have an important role to play, the conventional radiograph remains fundamental to the diagnosis of joint disease and is commonly the first imaging investigation undertaken. 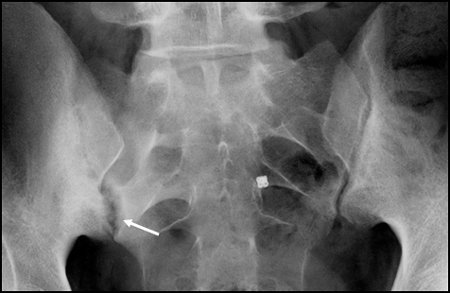
In cases of peripheral arthritis involving the small joints of the hands and feet, the distribution of joint disease detected on the radiograph is often as important in making the correct diagnosis as the radiographic features of the disease. The pattern of joint involvement in each case is particularly important, with consideration of the number of joints involved, whether or not the joints are affected symmetrically on both sides of the body, and which specific joints are affected. However, to accurately diagnose the underlying cause of a patient’s arthritis, consideration must be given to the clinical information available as well as to the imaging features of the disease. Imaging plays an important role in the diagnosis and management of joint disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
